Our Split Billing system enables hospitals to manage only one inventory and maximize 340B savings. Our solution is wholesaler, supplier, and IT system-neutral.

The SunRx Split Billing solution virtually separates 340B, non-340B, and GPO purchasing transactions in mixed-use settings to help ensure patient eligibility compliance, thereby allowing hospitals to manage only one physical inventory for all drugs dispensed within the hospital. With compliance in mind, the entire reporting suite is built around HRSA guidelines.
Split Billing Features
Our Split Billing system is a cloud-based tool that allows Covered Entities to create replenishment orders for outpatient and inpatient settings and track purchases within the entire pharmacy supply chain with auditable reports.
340B Contract Pricing
We ensure 340B contract pricing is honored and offer a comprehensive Medicaid validation process.
Unique Reconciliation
Our unique reconciliation process ensures that drugs not received by the hospital are added back to the 340B accumulator, thus recapturing the lost savings.
CDM-to-NDC
We build and maintain your CDM-to-NDC crosswalk.
SunRx Split Billing
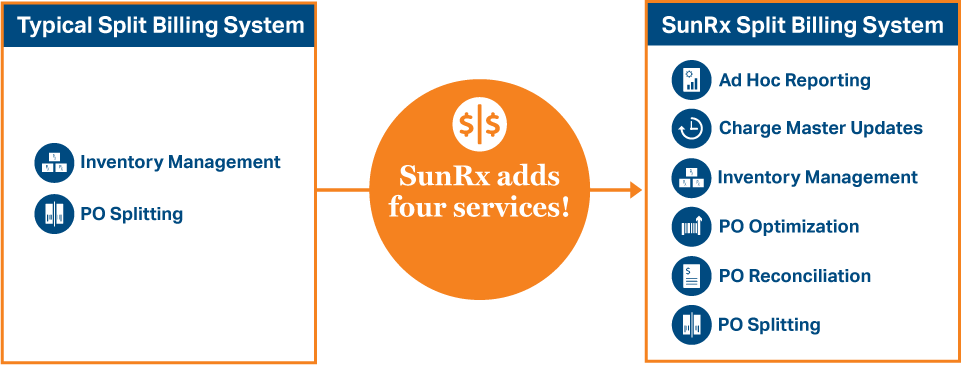
SunRx adds four additional services for the most robust 340B Split Billing Solution. The SunRx split billing solution includes:
Inventory Management, PO Splitting, PO Optimization, PO Reconciliation, Charge Master Mapping, and Ad–Hoc Reporting.
Virtual Inventory System
The Virtual Inventory System is an automated system that manages the flow of inventory, information and payments between Covered Entities, pharmacies and wholesalers. It is HIPAA & HITECH compliant.
Compliance
Maintains compliance against “diversion” and “Medicaid duplicate discounts”
Inventory Control
Allows contract pharmacies to dispense their own stock without the need to keep a separate 340B inventory.
Efficiency
Automates reporting and auditing requirements and reduces paperwork.

Learn more about our complete 340B solution. Ready for a change?

