In this series, SunRx offers and presents a brief overview on 340B solutions and services for consideration in the management of your 340B strategy. These on-demand videos aims to offer valuable insights to aid decision-making, compliance and optimize your 340B pharmacy program.
Watch: Manufacturer Mandate Management (M3)
Presented by Justin Ott from AuthorityRx
Watch: Advanced Claims Capture
Presented by Justin Ott from AuthorityRx
Watch: Supporting HRSA Audits
Presented by Justin Ott from AuthorityRx

- CEO, CFO, and COO
- Pharmacy Leaders
- Finance Leaders
- 340B Team Members
- Anyone interested in learning about 340B
Watch: Manufacturer Mandate Management (M3)
Presented by Justin Ott from AuthorityRx
Watch: Advanced Claims Capture
Presented by Justin Ott from AuthorityRx
Watch: Supporting HRSA Audits
Presented by Justin Ott from AuthorityRx

- CEO, CFO, and COO
- Pharmacy Leaders
- Finance Leaders
- 340B Team Members
- Anyone interested in learning about 340B
Claim Capture by Provider Type: A Compliance and Maximization Guide
 Industry Insights
Industry Insights
This article will discuss the importance of maintaining accurate provider panels and applying appropriate capture logic based on provider type.
Understanding Provider Panels
Provider panels are lists used by 340B Third-Party Administrators (TPAs) to determine which providers' claims are 340B eligible. At a minimum, a provider panel should include:
- Provider's eligible start date and National Provider Identifier (NPI)
- Service areas they are associated with
- Provider type
CEs must consistently maintain their provider panel to reflect changes in provider status.
Provider Types and Capture Logic
Accurately categorizing providers by type is essential for applying the appropriate claim capture logic. Here's a breakdown of common provider types and their implications for claim capture:
- Exclusive/Standard Providers: These providers are contracted by the CE and only practice within the CE's eligible service areas. They are expected to adhere to the CE's policies and procedures (P&Ps). Claims from exclusive providers can typically follow a capture logic that captures all scripts written with associated visits, as long as other eligibility criteria are met.
- Non-Exclusive/Non-Standard Providers: These providers are contracted by the CE but practice both within and outside the CE's eligible service areas. This could include ineligible service areas within the CE or facilities not affiliated with the CE. Due to their varying practice locations, claims from non-exclusive providers require capture logic that differentiates between eligible and ineligible facilities. Manual claim capture options, such as review queues or fallout reviews, can help maximize capture for this provider type.
- Referral Providers: These providers see patients referred from the CE but do not practice within the CE's eligible service areas. Claims from referral providers may be eligible for capture if they meet the CE's referral capture criteria outlined in their P&Ps. Capture logic for referral providers must track patient care through encounter data and referral notes. Like non-exclusive providers, manual capture options can be beneficial for referral providers.
Benefits of Distinguishing Provider Types for Claim Capture
Implementing capture logic by provider type is crucial for several reasons:
- Compliance: Ensuring that claims are captured according to the correct provider type is essential for maintaining 340B program compliance.
- Capture Maximization: By accurately categorizing providers and implementing appropriate capture logic, CEs can maximize their 340B benefit.
- Resource Optimization: Utilizing provider type-specific capture logic can reduce the strain on resources by minimizing unnecessary manual review of claims.
Next Steps for Your Organization
To ensure a compliant and maximized 340B program, consider the following steps:
- Review: Assess the accuracy of provider types associated with your 340B program.
- Verify: Confirm that an internal procedure exists for maintaining the accuracy of your provider panel.
- Collaborate: Contact your TPA to understand your provider type and capture logic options and ensure appropriate configuration within their system.
By understanding the nuances of provider types and implementing appropriate claim capture strategies, Covered Entities can ensure both the compliance and financial success of their 340B programs.
SunRx is here to help you simplify 340B program administration. Count on us to be your trusted 340B partner.
Our 340B Solutions include:
- Contract Pharmacy
- Uninsured 340B Prescription Discount Card
- Specialty Pharmacy
- Referral Capture
- Advanced Claims Capture
- Split Billing
Download our SunRx Solutions Brochure

To learn more, contact Stephanie Blaskoski.
Stephanie Blaskoski, 340B ACE
Team Lead, Account Management
SunRx
(858) 209-0010
sblaskoski@sunrx.com
The content in this blog is for informational purposes only and is not intended to be used in place of regulatory guidance. The opinions and views expressed herein are those of the authors and do not necessarily reflect the official position or opinions of SUNRx or any regulatory authority. Furthermore, some content may contain copyrighted material, the use of which has not always been specifically authorized by the copyright owner, but which we believe constitutes a "fair use" of any such copyrighted material as provided for in Section 107 of the US Copyright Law. We are making the information herein available in our efforts to advance understanding of the 340B program and its offerings. These views are always subject to change, revision, and rethinking at any time and may not be held in perpetuity.
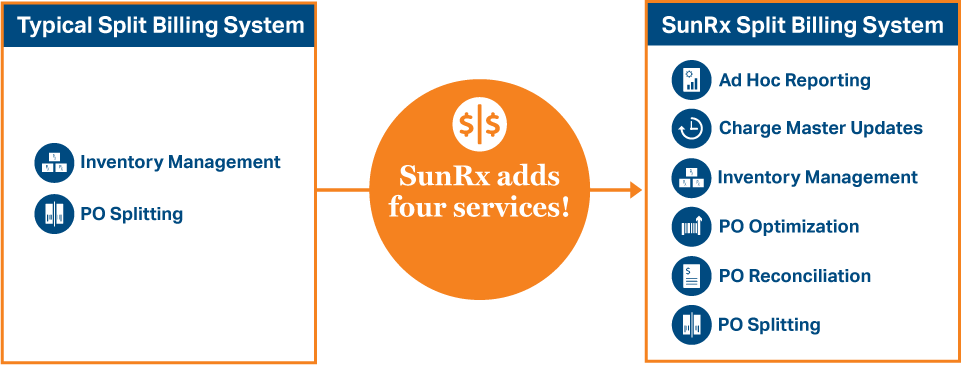
SunRx Split Billing
SunRx adds four additional services for the most robust 340B Split Billing Solution. The SunRx split billing solution includes:
Inventory Management, PO Splitting, PO Optimization, PO Reconciliation, Charge Master Mapping, and Ad–Hoc Reporting.
![]()
A Bold Suite of Solutions Built for a Dynamic Market
Each solution in the Command340B suite addresses a distinct market challenge. Together, they help covered entities reduce risk, protect savings, and strengthen program outcomes.

Advanced Claims Capture
ACC identifies and resolves eligible claims at risk of lost savings, maximizes results with fewer resources, and includes ongoing compliance support, delivering
results in days — not months.

ESP & Rebate Data Submission
The real-time data engine that integrates EHR, eligibility, ESP, and Beacon rebate submissions — streamlining validation and easing cash-flow strain.

Rebate Model TPA
Built for today’s rebate era, Edge organizes claim-level Beacon data and dual workflows — providing a unified view to manage rebate-based contracts.

Transparency Reporting
Aggregates Beacon savings and submission data into standardized transparency reports — helping entities meet manufacturer mandates and ensure compliance.

Compliance
Compiles Beacon data into a single tool for documentation, gap detection, and audit readiness — reducing workload and strengthening compliance.

Pharmacy Gateway
Connects and consolidates 340B data across sources — helping pharmacies seamlessly track, manage, and report both traditional and rebate program activity.

Take command and of 340B with SunRx!

Advanced Claims Capture
ACC identifies and resolves eligible claims at risk of lost savings, maximizes results with fewer resources, and includes ongoing compliance support, delivering
results in days — not months.

ESP & Rebate Data Submission
The real-time data engine that integrates EHR, eligibility, ESP, and Beacon rebate submissions — streamlining validation and easing cash-flow strain.

Rebate Model TPA
Built for today’s rebate era, Edge organizes claim-level Beacon data and dual workflows — providing a unified view to manage rebate-based contracts.

Transparency Reporting
Aggregates Beacon savings and submission data into standardized transparency reports — helping entities meet manufacturer mandates and ensure compliance.

Compliance
Compiles Beacon data into a single tool for documentation, gap detection, and audit readiness — reducing workload and strengthening compliance.

Pharmacy Gateway
Connects and consolidates 340B data across sources — helping pharmacies seamlessly track, manage, and report both traditional and rebate program activity.
![]()
A Bold Suite of Solutions Built for a Dynamic Market
Each solution in the Command340B suite addresses a distinct market challenge. Together, they help covered entities reduce risk, protect savings, and strengthen program outcomes.




